Amazing service provided with highly professional people. All doctors and nurses were very helpful in explaining everything and were very skilled. HIGHLY RECOMMEND!
What is (Periodontal) Gum Disease?
There are two types of gum disease. Gingivitis, which is familiar to people and is more common, is a condition that causes gums to become swollen, red, and bleed easily. Gingivitis is most commonly caused by inadequate brushing and flossing.
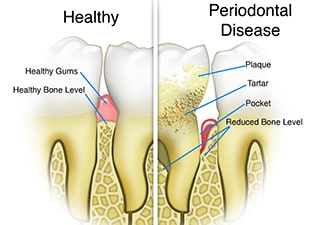 However, left untreated, Gingivitis can progress to Periodontitis. This is where plaque spreads below the gum line. Bacteria will collect there and release toxins. The body responds to the constant presence of toxins with chronic inflammation. This inflammation breaks down the tissue under the gum line, creating “pockets” which can then become infected. Over time, both gum tissue and bone are damaged or destroyed, which can eventually result in tooth loss.
However, left untreated, Gingivitis can progress to Periodontitis. This is where plaque spreads below the gum line. Bacteria will collect there and release toxins. The body responds to the constant presence of toxins with chronic inflammation. This inflammation breaks down the tissue under the gum line, creating “pockets” which can then become infected. Over time, both gum tissue and bone are damaged or destroyed, which can eventually result in tooth loss.
Gingivitis and periodontitis are often not painful at all. People will often ignore the inflammation or other symptoms until they come into the office wondering why they have a loose tooth. This is why it is very important to educate patients about gum disease, and why dentists will check the health and condition of the gums as well as the teeth at each checkup visit.
Gum disease is ultimately caused by two things: 1. the presence of bacteria in the mouth and 2. places for that bacteria to congregate and stay. Most often, bacteria collect on buildup (calculus) around and below the gum line.
Other conditions or factors that contribute to gum disease include:
Genetics (the tendency towards gum disease may be passed down through genes)
Poor or inconsistent oral hygiene habits at home, including not flossing frequently enough
Food stuck in the gums frequently (may be due to infrequent flossing or issues with crooked teeth or malocclusion)
Mouth breathing and snoring (may lead to severe drying of the gums and teeth in front of the mouth)
Dietary deficiencies, particularly in Vitamin C
Smoking or the use of tobacco products
Autoimmune or systemic diseases
Diabetes
Hormonal changes in the body including pregnancy
Bruxism (incessant clenching and grinding of the teeth)
Certain medications or medical treatments such as chemotherapy
Left untreated, gum disease will ultimately result in the loss of teeth. The gums and surrounding bone become so weakened by the bacteria and immune response that they will no longer be able to hold in the teeth. Furthermore, studies have directly connected the presence of oral bacteria associated with gum disease with heart disease. A healthy mouth truly can help lead to a healthy body. This is yet another reason why proper diagnosis and treatment of gum disease is very important.
Untreated gum disease can result in the loss of teeth, but it doesn’t just stop there. Gum disease can have major impacts on other body systems and has been tied to other serious health issues, and can make certain existing conditions worse. Other areas of the body directly affected by gum disease include the heart, lungs and respiratory system, reproductive system and pregnancy for women, digestive system, and more. Get more information about how Gum Disease affects the whole body.
The most common procedure used to treat gum disease is called Scaling & Root Planing (SRP). This is typically done on one quadrant, or quarter, of the mouth, at a time.
First, your dentist or dental hygienist will numb the area to be treated. Then your dentist or hygienist will perform a deep cleaning (scaling) to remove calculus (build-up) underneath the gum line, all the way to the roots of the teeth. This also removes the bacteria that are causing the infection. Your dentist may also smooth down areas of the root (planing) to prevent bacteria from finding places to collect in the future.
Gum disease can be reversed in most cases when proper care is taken. Plaque control consisting of professional cleanings at least twice a year accompanied by daily brushing and flossing is absolutely necessary. Brushing eliminates plaque from the surfaces of the teeth that can be reached, while flossing removes food particles and plaque from in between the teeth and under the gum line.
The cost of treating periodontal disease will vary depending upon a variety of factors, including the severity of the condition, the area(s) needing treatment, the type of treatment provided, and the amount of follow up needed to ensure the treatment is successful. Prior to your procedure, your dentist will review what treatment is needed, and our staff will provide you with information about any fees associated with the procedure, as well as options available to help make sure your receive the dental care you need in a way that fits into your budget.
If you have dental insurance, your coverage may include treatment for periodontal disease. It is important to stay up to date with your insurance coverage. Our staff is happy to review your coverage with you to ensure you are maximizing your insurance benefits while minimizing any out of pocket expenses.
Early symptoms of gingivitis include red, swollen gums which may present in one specific area of the mouth. Your gums may bleed infrequently, or they may bleed often when you brush or floss. Symptoms of more advanced gum disease can include bad breath that does not go away after brushing or rinsing, sore, bleeding gums, or loose teeth.
Your teeth may look longer because your gums have receded. If you have a partial, it may fit differently, or your teeth may not bite together normally. If you experience these symptoms, it is best to see your dentist as soon as possible.
Where can I get evaluation or treatment for gum disease
All 1st Family Dental offices offer evaluation and treatment for periodontal disease as a part of our comprehensive oral health services.
Preparation and Post-procedure care for gum disease treatment
Many patients may experience some degree of sensitivity in the treated area, but this should go away after a short period of time. Your dentist will review post-procedure care instructions which include avoiding smoking and avoiding certain foods and beverages for a period of time.
After about 2 to 3 weeks, you should return to the office for a follow up visit to assess how the gums are healing, review at-home hygiene habits and techniques, and to determine next steps if additional treatment is necessary.
Patients who are curing gum disease will often need to return for more cleaning and “periodontal maintenance” visits, usually every 2 to 3 months for a period of time to ensure that the bacteria and calculus are not collecting below the gum line, and to help the healing process.
How can I prevent gum disease?
The majority of gum disease cases can be prevented by good oral hygiene at home and regular checkups every 6 months with your dental professional. A healthy oral hygiene routine consists of brushing for two minutes, twice a day with a soft-bristled brush and toothpaste, and flossing at least once per day. If you have been treated for gum disease in the past, your dentist may recommend a maintenance program requiring more frequent checkups and cleanings for a limited amount of time.
Catching issues such as gum disease as early as possible will help keep your body in prime condition to heal itself. With that in mind, it is also important to take good care of your whole body. A healthy diet, exercise, and regular check-ups with your general doctor will help you to ensure your mouth truly is the reflection of your good health.
Simple Steps to Getting Started

STEP TWO
Book An Appointment
What Patients are Saying About Us
I have just completed a 16 months orthodontic procedure. Very happy how much of a difference it is! I can smile with confidence! A truly high professional dental and orthodontic services by First Family Dental! Thanks to Dr. Abboud, Dr. Williams and all the staff at First Family Dental and Midwest Orthodontics that showed a genuine patient care…
Sam K.
This has been my go to dentist location since I can remember. I recently took my mom again after her crown fell off and I just can’t rave enough about this location and the dentist that helped us out! If you want the old school family vibe-this is the place to go to. No rip offs if anything they work with you and make you feel comfortable.
Emma M.
My appointment today was outstanding, from being greeted by name by the receptionist upon my arrival, through the cleaning process by Debbie and the dental exam. The equipment is all top shelf and the treatment rooms are very clean and comfortable. I would highly recommend 1st Family Dental in the Burr Ridge Village Center to anyone looking for an exceptional dental experience.
Tony T.
I prepared myself for a life without teeth, and did not think there was anything that could be done to help me. I expected to learn to live out the rest of my years hiding my smile, and living with my digestive problems – until I found 1st Family Dental.

Joe F.
Before I knew it, the assistant came out to tell me they were done and she did well. I was so relieved and happy. My daughter was happy and calm. I asked her about her visit. She now has no fears, and can’t wait for her next cleaning in 6 months.
Stef G.
When I got home and looked at my teeth in the mirror, I was astounded with the job that Dr. Akhikar had done. The new filings were much less noticeable than my previous one. I couldn’t have been more satisfied.
Henry B.
The staff was friendly and one of the assistants even let me hold her hand while the extractions were taking place! The dentist who treated me was very professional and made me feel very comfortable.
Cynthia E.
This dental office has provided me the best care and treatment out of any dentist I have ever visited… I have made them my primary dentist because it has taken me years to find a dentist I can trust.
Brittany M.
Previous
Next

